|
Gentle reminder for the day for those who have had a concussion – Don’t push through!
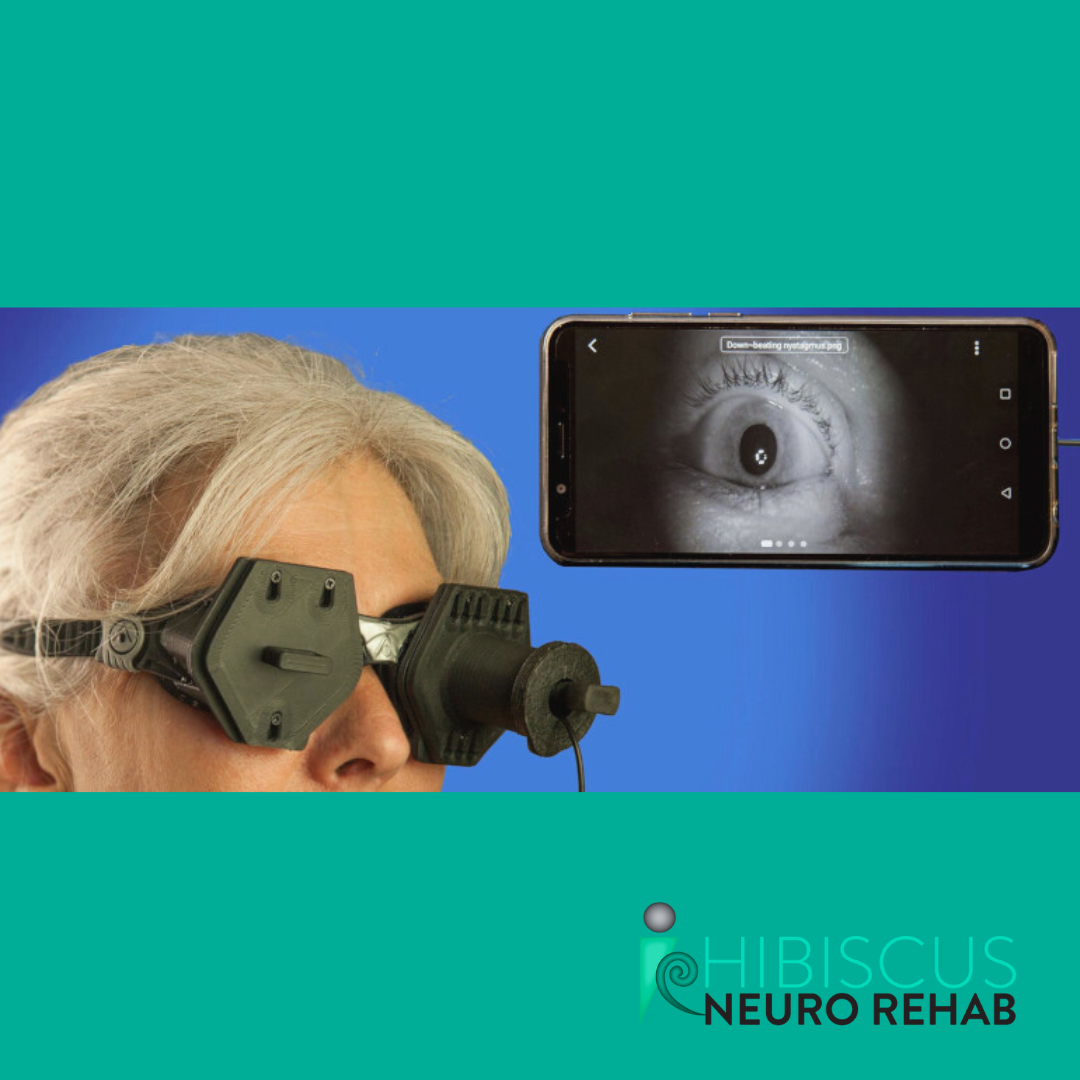
Remember that following a concussion the brain needs use more energy to manage normal daily functions than it did before your concussion ………AND it needs to be diverting a lot of its energy to help the healing process. Your brain has a finite amount of energy, and after it has diverted the energy required for helping with healing and repair there can often be little left in the way of reserves. Your job is to manage these reserves, and not push through your brain’s capabilities. If you do push through, you risk a symptom flare, which is never fun, and likely to then prevent you from being able to manage the things you had planned for the rest of the day. Remember your x3 P’s: 1. PLAN: your day and your week. Schedule in adequate breaks to help you recover and limit the risk of flaring your symptoms. 2. PRIORITORISE: Look at what needs to happen in your day/week. Prioritise what must absolutely be done, and what you can leave or do if your energy levels allow. 3. PACE: Spread more cognitive/physical/stressful tasks out over the week, plan breaks around these. Listen your body’s feedback when doing any task, and pace yourself, when you start to feel the signs that you might get symptomatic, stop and break to prevent your symptoms flaring. In the early stages of your concussion recovery this will be a lot of trial and error. You need to respect what your body is signalling to you, and not push through. When you come into clinic and your vestibular system is affected (i.e. your inner ear), chances are that we may use our vesticam as part of our assessment! The vesticam are infrared goggles that allow us to see a live video of your eyes while we do testing.
Benefits of using infrared goggles: - Accurate assessment due to clients not being able to fixate their vision (which can suppress any underlying vestibular pathologies). - Better able to see any nystagmus (rapid oscillations/flicking of eyes) present that may indicate certain vestibular or central pathologies present. - Reduces risk of missing a potential diagnosis of pathology present. These are extremely beneficial for both clients and therapists to use to maximise assessment time and therefore improve the specificity of treatment for the client. So often we have clients come in for an assessment for their vertigo and report that they have been trying to do the EPLEY maneuverer themselves at home (often repetitively each day) and it hasn’t been helping them.
The Epley maneuverer is a specific canal repositioning treatment maneuverer to treat BPPV in either the right or the left posterior semi-circular canal. The Epley can only be effective when it is used to treat the correct canal. In the inner ear we have 6 semi-circular canals, 3 on the right, and 3 on the left. Before the Epley is used to treat BPPV it’s really important that you are assessed first - to determine that you actually have BPPV, and then to establish which canal the BPPV is in. If you do not know which canal the BPPV is in, then the Epley may not help to treat the BPPV or resolve your vertigo. There is also a risk that you can worsen your BPPV by shifting the crystals into another or multiple canals. It is also important to also consider that your symptoms of vertigo or dizziness is not always a result of BPPV! Before undertaking any treatment it is really important to have an assessment to determine the root cause of your symptoms. Doing vestibular/vertigo treatments can provoke your symptoms more and can be traumatic for people - an experienced therapist can talk you through exactly what is happening and why you are experiencing your symptoms, and provide ongoing reassurance that you are safe when your body and symptoms tell you otherwise. Once a diagnosis of BPPV has been established your vestibular therapist will then be able to prescribe any further canal repositioning manoeuvres to do at home, and give you individualised instructions on how to specifically for your BPPV. Please get assessed for BPPV before you start doing the Epley at home! As we get older, our muscle strength reduces and there can be changes in our balance, mobility and fitness.
In the presence of adequate exercise, these changes in muscle strength and fitness with age are substantially attenuated. Exercise is a preventive strategy for many chronic diseases, including cardiovascular disease, stroke, diabetes, osteoporosis, and obesity; improvement of mobility, mental health, and quality of life; and reduction in mortality, among other benefits. Exercise intervention programmes improve the hallmarks of frailty (low body mass, strength, mobility, physical activity level, energy) and cognition, optimising functional capacity during ageing. Here are the recommendations for older adults who are 65 years and older, being that of 150 minutes moderate cardio training each week, plus 2 strength trainings per week (according to the WHO's global recommendations). Remember that exercise should be individual to you, as everyone has different health conditions or circumstances, so this may need to be altered accordingly. If you are unsure or need help devising an appropriate programme, please contact us so we can help you! For those who are interested, there is a great article (Expert Consensus Guidelines) that summarises recommendations according to various circumstances, including if you want to improve bone density specifically or help increase lean mass, for example, and discusses different modalities for each circumstance. Izquierdo, M., Merchant, R.A., Morley, J.E. et al. International Exercise Recommendations in Older Adults (ICFSR): Expert Consensus Guidelines. J Nutr Health Aging 25, 824–853 (2021). Walking is often the number one goal that clients want to improve following stroke. Emphasis is often on the walking pattern or how the walking looks. Optimising the walking pattern after stroke is important to improve walking safety and efficiency, energy conservation and improve overall performance. However an important feature of walking that is often be overlooked is walking speed.
Studies have shown that walking speed is reduced by up to 50% following a stroke which limits participation in day to day activities, socialisation and the ability to walk in the community. This can lead to individuals becoming housebound, socially isolated and dependant on others for extra supports. Nascimento et al 2015 did a systematic review of 7 clinical trials which looked at training walking speed following stroke using external cues with setting cadence. The cadence/speed of stepping was set using a metronome app. The individuals in the trials were tasked to match their steps to the beat of the metronome which was progressively increased. The results of these trials showed that cueing walking speed using a metronome increased walking speed by 50%, by training for 30minutes a day over a 4 week period. This is just one example of a cost- effective tool to help retrain walking speed. If you would like more help on how you can improve your walking and get your pace up with your walking post-stroke then get in touch with us. It can get tougher in these colder months to keep going. Or perhaps you are wanting to start working towards a goal, but know that you find it tough staying motivated or don't know where to begin.
Here are 9 tips to consider when starting a new journey, be it in exercise, nutrition or something completely different. 1. Knowing your 'why': Knowing WHY you started this journey and WHY you are doing it can help keep you in check and keep you motivated to carry on when it gets tough. What is your WHY? 2. Start small: When working on a life long change, start with small, achievable changes so that you are less likely to give up and you can stay motivated as you achieve these tasks. 3. Set a date: Giving yourself a realistic deadline to achieve goals can motivate you to get working and not give up! You will feel accomplished when you achieve this goal by this date. 4. Checklist: These are GREAT for 2 reasons:
6. Find a mentor: Finding someone who is knowledgeable in the field that you are interested in and working towards can help ensure your goals are realistic and provide you with insight into how to achieve your goals safely and efficiently. 7. Find a routine: Once you know what your goals are and know your WHY, setting up a consistent routine every day or week will help your mind and body adjust to these changes. Consistency is key. 8. Be around the right people: Surround yourself with people who will support you and motivate you to keep going. Choosing who you give your energy to will have a huge impact on your end goal and motivation levels. 9. Celebrate all wins: No matter how big or small, celebrate EVERY win. Acknowledge these wins and be proud of the progress you have made. Remember these wins and use this as fuel for your motivation! Let us know if you have tried any of these tips, and how have they worked for you? CONCUSSION MYTHS vs REALITY
So often we get clients who come see us very late after having a concussion, and report to us that they were told to only rest, or to just carry on with their everyday activities. When we talk to them, they can report still feeling fatigued, having sleep issues and/or can't handle doing a lot of exercise, to name a few. Research now supports that pure rest is actually doing a dis-service to those with concussion, and that graduated return to activity after 24-48 hours of physical and cognitive rest (monitored by a health professional with concussion experience) is favored in concussion recovery. Graduated activity can help with: Increasing blood flow, and therefore oxygen to the brain to help promote healing Improving mood and cognition Increasing your exercise tolerance again Promoting neuroplasticity (brain changes to promote healing and creating new neural pathways) It is important to note that a large benefit of reaching out to a qualified health professional in concussion management is for education and guidance around pacing strategies, fatigue management and the most recent evidence-based approaches to concussion management. Concussion rehab is very individual and is not a "one size fits all" approach. If you recently had a concussion, or are experiencing ongoing symptoms that are not resolving, please contact us so we can help you. Did you know that vestibular migraine is now considered one of the most common vestibular Disorders?? It affects 1-2.7% of the general population and 11% of patients who attend a specialized dizziness clinic. (Shen et al 2020) Vestibular migraine is a clinical syndrome of transient episodic vertigo/dizziness, or unsteadiness. It can last seconds to hours, in some cases lasting for several days. It includes features of temporary vestibular dysfunction such as nausea, dizziness, nystagmus, imbalance and at times falls. Following a Vestibular migraine an individual may feel symptoms of fatigue, brain fog, poor concentration, imbalance, motion sensitivity, nausea, and in some instances have continuous light headedness. 30% of individuals with vestibular migraine will have no associated migraine before or after the episode of vertigo/dizziness. Diagnostic criteria for Vestibular MigraineA. At least five episodes of significant dizziness/vertigo lasting from minutes to days B . A current or past history of migraine C. At least half the episodes of vertigo have one or more migrainous feature associated with them such as typical migraine headache (one sided location, pulsating quality, moderate or server pain intensity, aggravation by routine physical activity, photophobia/photophonia, or visual aura) D. Not better accounted for by another vestibular or headache diagnosis (Simplified from the International Headache Society Classification of Headache ICHD-3-Feb 2018) Treatment of vestibular migraineManagement of Vestibular migraine requires identification of the main triggers for the migraine, assessing for the vestibular and functional issues that arise due from the migraine, then taking a multi-modal approach to management, combining:
Here are some cognitive dual tasking ideas that you can try. These have been used in research studies and we often use these ideas in our clinic to train dual tasking, particularly in balance and walking training.
Randomly naming numbers between 100 and 500 (without repetition or consecutively) Randomly naming odd (or even) numbers between 1 and 100 (without repetition or consecutively) What is it?
Peripheral neuropathy refers to the many conditions that result in impairment to the peripheral nervous system (PNS). The role of the PNS, which is a vast communication network within our body, is to relay information between the central nervous system (the brain and spinal cord) and all other parts of the body. Peripheral nerves send different types of information to the central nervous system, including pain, temperature, touch, proprioception and pressure, to name a few. There are 3 main types of nerves that can be affected in the PNS: |
�
Categories
All
Archives
July 2023
|
|
Contact Us
Give us a call or send us an email to find out how we can help you on your rehab journey Phone 09 424 3254 office@hibiscusneurorehab.co.nz Visit us @ HEALTH HUB 3/55 Karepiro Drive, Stanmore Bay, Whangaparaoa |
Cancellation Policy:
Out of courtesy to your therapist, and other clients who may be waiting for an appointment, please inform us of cancellations as soon as possible.
Cancellations Charges: Short notice cancellations within 48 hours of your appointment or reschedules will incur a late cancellation fee of 60%.
For block bookings, one session will be deducted for three cancelled appointments.
Please be aware that ACC does not cover all cancelled appointments.
How to Cancel Your Appointment
If you need to cancel your appointment, please call us at 09 424 3254 between the hours of 8am – 5pm. If necessary, you may leave a detailed voicemail message. We will return your call as soon as possible.
Late Cancellations/No-Shows
A cancellation is considered late when the appointment is cancelled less than 48 hours before the appointed time. A no-show is when a patient misses an appointment without cancelling. In either case, we will charge the patient a 60% missed appointment fee.
Out of courtesy to your therapist, and other clients who may be waiting for an appointment, please inform us of cancellations as soon as possible.
Cancellations Charges: Short notice cancellations within 48 hours of your appointment or reschedules will incur a late cancellation fee of 60%.
For block bookings, one session will be deducted for three cancelled appointments.
Please be aware that ACC does not cover all cancelled appointments.
How to Cancel Your Appointment
If you need to cancel your appointment, please call us at 09 424 3254 between the hours of 8am – 5pm. If necessary, you may leave a detailed voicemail message. We will return your call as soon as possible.
Late Cancellations/No-Shows
A cancellation is considered late when the appointment is cancelled less than 48 hours before the appointed time. A no-show is when a patient misses an appointment without cancelling. In either case, we will charge the patient a 60% missed appointment fee.









 RSS Feed
RSS Feed
